Maxillofacial (Jaw) Surgery, San Antonio, TX
Have you ever seriously considered the critical role your jaw plays in daily living?
A small or abnormally shaped jaw can contribute to dental problems, bite issues, airway obstruction, obstructive sleep apnea, and aesthetic imbalance. Jaw surgery, also called maxillofacial surgery, improves the functionality and appearance of the lower face and jawline. It is also an effective treatment option for sleep apnea.
Maxillofacial surgery is very complex, requiring a deep understanding of facial anatomy and mastery of surgical techniques to properly execute. Given their critical role in your long-term happiness and well-being, facial features and sleep health should be trusted only to a world-class surgeon.
Dr. Jose Barrera’s 30 years of maxillofacial surgery experience began at Stanford University with training from the renowned experts in jaw surgery, Drs. Robert Riley and Nelson Powell. He is board-certified in facial plastic and reconstructive surgery, as well as fellowship-trained in maxillofacial surgery, facial plastic and reconstructive surgery, sleep medicine and sleep surgery. He served as Chairman of Otolaryngology-Head and Neck Surgery at San Antonio Military Medical Center, and as an Assistant professor at Stanford University, Adjunct Associate Professor at Texas Health Sciences Center in San Antonio, and Clinical Professor at the Uniformed Services University in Maryland.
Dr. Barrera is an avid researcher, advancing the knowledge and techniques used in the aesthetics and sleep medicine fields with more than 70 published medical papers. He now brings his impeccable surgical skill and aesthetic sensitivity to patients at Texas Center for Facial Plastic and Laser Surgery.

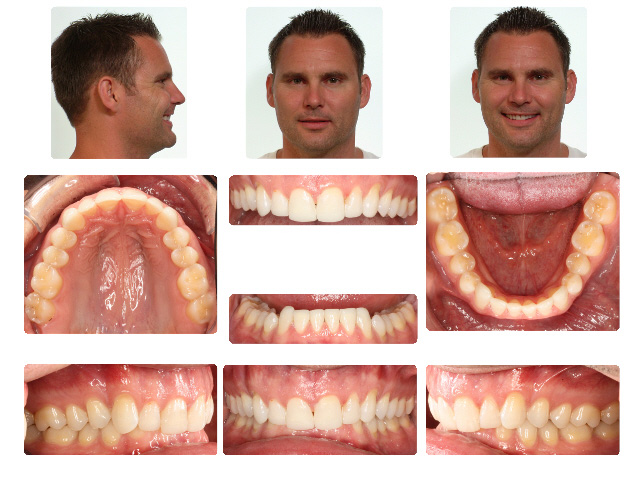
Dr. Barrera works with a team of orthodontists, prosthodontists, and dental sleep medicine experts from around Texas. From his backyard in San Antonio to McAllen, Austin, Dallas, Houston, and Laredo, or out of state in the United States, Dr. Barrera will work collaboratively with your referring dentist. Could you benefit from a jaw surgery consultation with Dr. Barrera? Call Texas Center for Facial Plastic and Laser Surgery at 210-468-5426 to get your specific questions answered or schedule a consultation at our San Antonio plastic surgery practice.

What Is Maxillofacial Surgery?
Jaw surgery seeks to correct irregularities in the jaw and tooth alignment. These corrections often improve the airway, allowing patients to breathe easier. In many cases, there is a significant reduction in sleep apnea symptoms. Dr. Barrera uses many different techniques for jaw surgery including:
- Maxillary impaction
- Mini-implant “assisted” rapid maxillary expansion (MARPE)
- Surgically assisted rapid maxillary expansion (SARPE)
- Maxillary Mandibular advancement surgery (MMA)
- LeFort I osteotomy
- Genioglossal advancement (GA) surgery
- Bilateral sagittal split-ramus osteotomy
- Sliding genioplasty
- Simultaneous rhinoplasty with maxillary surgery
- Uvulopalatopharyngoplasty and pharyngoplasty
- Tonsillectomy
- Mandibular sagittal split osteotomy
- Chin and jaw reduction
Dr. Barrera is highly experienced with these techniques and many others, using maxillofacial surgery to improve the airway, enhance aesthetics, and treat sleep apnea.
During your consultation, Dr. Barrera will outline his recommendations for treatment and help you to understand the benefits you’ll personally experience from this procedure. As one of San Antonio’s top facial plastic and reconstructive surgeons, Dr. Barrera is uniquely qualified to provide maxillofacial surgery for sleep apnea and other medical conditions. He often uses a phased approach, using simpler and less invasive surgeries initially and scaling up to more advanced surgeries if the initial treatment phases are unsuccessful.


Maxillofacial Surgery for Sleep Apnea in San Antonio
Maxillofacial surgery can dramatically reduce the symptoms of sleep apnea, a sleep disorder where patients intermittently stop breathing during the night. For many of our patients, maxillofacial surgery provides relief from sleep apnea without the use of a CPAP.
How does jaw and palate surgery improve sleep apnea? Jaw abnormalities can create airway obstructions. During sleep, these obstructions may be compounded by blockages from soft tissues including the palate, tongue, tonsil, and pharyngeal walls. Many patients have more than one point of obstruction.
Maxillofacial surgery for sleep apnea repairs the jaw and soft tissues to alleviate breathing obstructions and open the airway. With sleep apnea symptoms alleviated, quality of life improves. Patients with untreated sleep apnea are at an increased risk for diseases like heart disease, diabetes, and stroke. Many experience difficulty working or safely operating a motor vehicle, due to an increased likelihood of suddenly and unintentionally falling asleep.
The underlying skeletal foundation, the airway, and its encompassing soft tissue have a complex and dynamic relationship. To ensure that your treatment is effective, Dr. Barrera may order a sleep study, upper airway endoscopy, clinical evaluation, or Drug-Induced Sleep Endoscopy (DISE). Testing provides Dr. Barrera with the information he needs to create a comprehensive and effective treatment plan.
Dr. Barrera is Board Certified in Facial Plastic and Reconstructive Surgery. He has earned board certification in Otolaryngology – Head and Neck Surgery and Sleep Medicine and now actively teaches fellows as a fellowship director with the American Academy of Facial Plastic and Reconstructive Surgery. He is also double fellowship trained in Facial Plastic Reconstructive Surgery and Sleep Surgery making him a top expert in sleep medicine in Texas.


Jaw Surgery Frequently Asked Questions
Learn more about jaw surgery at a consultation with Dr. Barrera. He can help you explore your options and determine if you’re a good candidate for surgery. Many patients with sleep apnea can benefit from surgical correction of airway blockages.
Maxillofacial surgery for sleep apnea is an effective treatment option for many patients with obstructive sleep apnea. This procedure can open the airway and remove obstructions, eliminating or dramatically improving the occurrences of breathing disruption during sleep.
If you have sleep apnea and are looking for surgical solutions, come see Dr. Barrera. After a sleep study, physical examination, and other screenings, he can help you determine if surgery is an effective choice. Dr. Barrera has a success rate of over 90% in patients undergoing maxillary mandibular advancement surgery (MMA), a type of maxillofacial surgery.
Dr. Barrera uses many different surgical techniques to treat sleep apnea and improve the function and appearance of the jaw. Costs vary widely depending on the techniques and procedures needed for treatment. We’ll provide detailed cost information at your consultation.
Many patients experience cosmetic benefit from their maxillofacial procedures; however, it is important to remember that aesthetic beauty is complex and variable. We treat many patients with jaw measurements that fall outside of the normal spectrum that are strikingly beautiful. The opposite is also true. Some patients with perfect jaw measurements may feel unhappy with their facial appearance. As you work with Dr. Barrera in preparation for your surgery, we can discuss the aesthetic changes you’ll experience with maxillofacial surgery. If the jaw condition is a birth defect, congenital deformity, or acquired from abnormal dentition or trauma, the aesthetic and functional goals will be discussed during the consultation. Some aesthetic changes such as changes to the nasal tip projection or rotation may require a staged secondary rhinoplasty surgery after the maxillofacial surgery. The complex nature of craniofacial surgery is managed by one or more operations to achieve desired results, improved symmetry, and aesthetic balance.
Dr. Barrera’s extensive experience in plastic and reconstructive surgery enables him to focus on both the aesthetics and function of the jaw. He uses physical examination, not solely x-ray, to determine the changes necessary to enhance physical beauty as well as jaw functionality. Our approach is always customized to a patient’s unique anatomy, ethnicity, and aesthetic preferences, never based solely on measurements in a textbook. Facial aesthetic photos, CT scan of the craniofacial skeleton, and a customized virtual plan are utilized for planning and executing maxillofacial surgery in Dr. Barrera’s practice.
Maxillofacial Surgery in San Antonio- Schedule Your Consultation with Dr. Barrera Today
Find relief from your sleep apnea, airway obstructions, and other jaw problems with maxillofacial surgery. Schedule your consultation with our board-certified plastic surgeon and sleep apnea expert Dr. Jose Barrera by calling 210-468-5426.



